Kidney Failure
Q1: Recently, my father had chronic renal failure at age 72. Does he need a lifelong dialysis?
 Kidney / Renal failure is divided into acute and chronic. When chronic kidney disease gradually deteriorates to the stage of requiring dialysis, the so-called fifth stage, i.e. end-stage renal failure, it means that patient’s kidneys are no longer able to excrete toxins out the body effectively, thus requiring a kidney function replacement therapy such as haemodialysis. Of course, this renal function replacement therapy is a long-term necessity for detoxifying the body of patient regularly.
Kidney / Renal failure is divided into acute and chronic. When chronic kidney disease gradually deteriorates to the stage of requiring dialysis, the so-called fifth stage, i.e. end-stage renal failure, it means that patient’s kidneys are no longer able to excrete toxins out the body effectively, thus requiring a kidney function replacement therapy such as haemodialysis. Of course, this renal function replacement therapy is a long-term necessity for detoxifying the body of patient regularly.
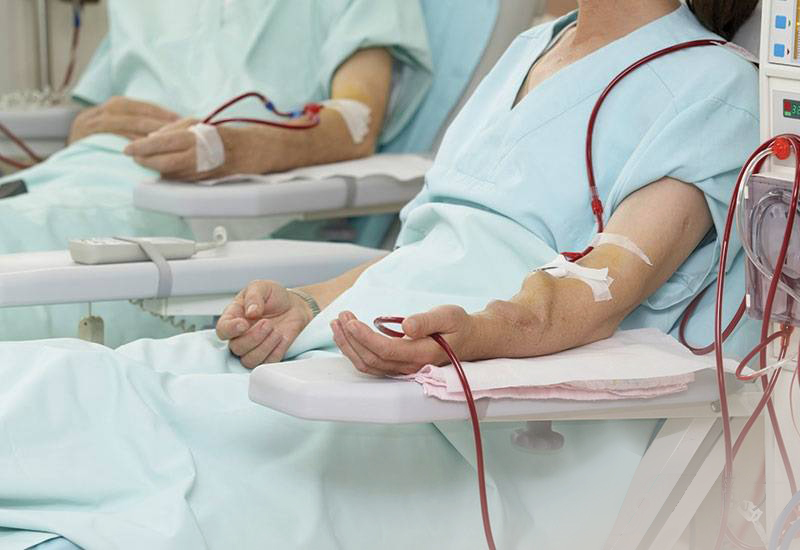

Q2: What are the restrictions on the diet after dialysis?
 Patients with early and mid-term kidney disease should take low-protein diets to reduce the burden of kidneys. However, patient must do some adjustment right after dialysis, because patient will lose some proteins during dialysis process. To avoid malnutrition, protein intake should be higher than before dialysis. Apart from this adjustment, patient should also obey low-intake of phosphorus, low-potassium and low-sodium foods. In addition, daily water consumption should not exceed 800 to 1000 cc per day.
Patients with early and mid-term kidney disease should take low-protein diets to reduce the burden of kidneys. However, patient must do some adjustment right after dialysis, because patient will lose some proteins during dialysis process. To avoid malnutrition, protein intake should be higher than before dialysis. Apart from this adjustment, patient should also obey low-intake of phosphorus, low-potassium and low-sodium foods. In addition, daily water consumption should not exceed 800 to 1000 cc per day.

Q3: What are the alternative treatments for kidneys?
There are three options for kidney replacement therapy:
- Hemodialysis: Use arteriovenous tubing to deliver blood to a dialyzer via a kidney hemodialysis machine, in order to achieve the efficacy of detoxification.
- Peritoneal Dialysis: Apply the peritoneum in the abdomen to achieve the efficacy of detoxification. It uses a special dialysate to inject into the abdominal cavity, and then drains out after 4 to 6 hours.
- Kidney transplant: Kidney donors can be classified as having a blood relationship or no blood relationship, and can also be divided into brain death donors and living donors.